Remote Patient Monitoring (RPM) continues to expand rapidly in 2026, becoming a key driver of both patient outcomes and provider revenue. However, to fully benefit from RPM programs, providers must understand RPM CPT codes, billing requirements, Medicare rules, and reimbursement rates.
This guide explains everything you need to know about remote patient monitoring CPT codes (99453, 99454, 99457, 99458) and how to bill them correctly.
What Are RPM CPT Codes? (Featured Snippet)
RPM CPT codes are billing codes used by healthcare providers to get reimbursed for remote patient monitoring services, including device setup, data transmission, and patient management. The main RPM CPT codes include 99453, 99454, 99457, and 99458.
What Are RPM CPT Codes?
Before diving into RPM billing requirements and Medicare rules, it is important to understand how these codes function within the broader remote patient monitoring reimbursement system.
Definition of Remote Patient Monitoring CPT Codes
Remote patient monitoring CPT codes are standardized billing codes that allow providers to report and receive reimbursement for services such as device setup, physiological data collection, and ongoing patient management.
These codes form the foundation of RPM billing under Medicare and commercial insurance plans.
How RPM Fits Into Medicare & Digital Health (2026)
In 2026, RPM is a core component of Medicare-supported digital health programs. Providers increasingly integrate RPM into chronic care management, telehealth services, and value-based care models to improve outcomes and generate recurring revenue.
Now that the basics are clear, the next important question is why RPM CPT codes play such a critical role in provider revenue.

Why RPM CPT Codes Matter (Revenue & Medicare Advantage)
RPM is not just a clinical tool—it is a scalable revenue model within modern healthcare systems.
Recurring Revenue from RPM Programs
RPM enables providers to generate predictable monthly revenue through billing codes such as 99454 for device monitoring and 99457 for care management time.
This recurring structure makes RPM one of the most reliable reimbursement models in outpatient care.
Alignment with Medicare Value-Based Care
According to CMS (Centers for Medicare & Medicaid Services), RPM supports proactive care by improving chronic disease management and reducing hospital readmissions. This aligns directly with value-based care incentives and long-term cost reduction strategies.
With a clear understanding of its value, the next step is identifying which RPM CPT codes are used in practice.
Complete RPM CPT Codes List (Medicare 2026)
Before breaking down each code individually, it is helpful to review the full list of commonly used RPM CPT codes.
Core RPM CPT Codes Table
| Code | Description | Frequency | Key Requirement |
|---|---|---|---|
| 99453 | Set up and patient education | One-time | Device onboarding |
| 99454 | Device supply and data transmission | Monthly | Minimum 16 days of data |
| 99457 | Treatment management (20 minutes) | Monthly | Interactive communication |
| 99458 | Additional time (20 minutes) | Monthly | Additional care time |
This table represents the core structure of remote patient monitoring billing codes under Medicare.
Most Common Code Combinations
In most RPM programs, providers commonly bill 99454 together with 99457. Additional time can be billed using 99458 when care exceeds the initial 20-minute threshold.
Understanding the list is only the first step. Accurate billing requires a deeper understanding of how each code works.
RPM CPT Codes Breakdown (99453, 99454, 99457, 99458 Explained)
To build an effective RPM billing workflow, each CPT code must be applied correctly.
CPT 99453 – Setup & Patient Education
This code is billed once per patient and covers device setup, onboarding, and patient education. It represents the starting point of any RPM program.
CPT 99454 – Device Supply & Data Transmission
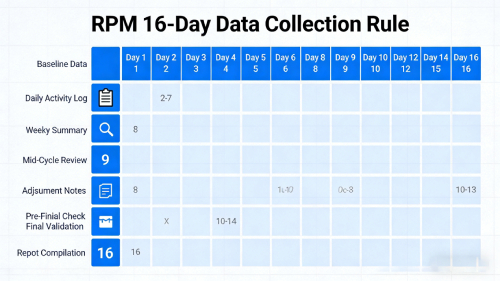
This is a monthly billing code that requires at least 16 days of data collection within a 30-day period. This requirement is often referred to as the RPM 16-day rule and is essential for reimbursement eligibility.
CPT 99457 Requirements (Featured Snippet)
CPT 99457 requires at least 20 minutes of clinical staff or provider time per month, along with real-time interactive communication such as phone or video with the patient.
CPT 99458 – Additional Time Billing
This code is used when monitoring and management exceed 20 minutes. Each additional 20-minute increment can be billed separately, allowing providers to increase revenue based on patient needs.
Even with a strong understanding of these codes, providers must follow strict billing requirements to ensure compliance.
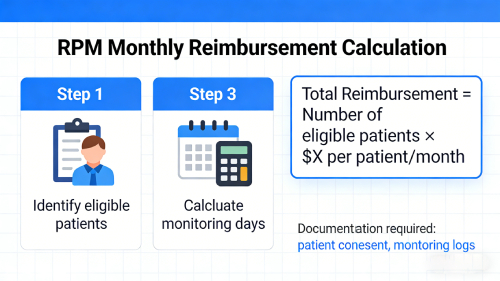
RPM Billing Requirements (Medicare Rules Explained 2026)
RPM billing is governed by CMS rules that define how and when services can be reimbursed.
RPM Billing Requirements (Featured Snippet)
RPM billing requirements include at least 16 days of data collection within a 30-day period, documented patient consent, time tracking for care management, and interactive communication between provider and patient.
RPM 16 Day Rule Explained
To bill CPT 99454, providers must collect physiological data for a minimum of 16 days within a 30-day billing cycle. Failure to meet this requirement will result in denied claims.
RPM Documentation Requirements (CMS Audit Checklist)
Providers must maintain proper documentation, including patient consent, device usage logs, time tracking records, and communication notes. These records are essential for compliance with CMS audit standards.
How to Bill RPM Medicare (Step-by-Step Insight)
Billing RPM under Medicare requires a structured process that includes patient enrollment, device setup, data monitoring, time tracking, and documentation of patient interaction.
Once billing requirements are clear, the next major consideration is reimbursement.
RPM Reimbursement Rates (Medicare 2026 Explained)
RPM continues to be widely adopted due to its strong reimbursement potential.
RPM Reimbursement (Featured Snippet)
RPM reimbursement typically ranges from $80 to $120 per patient per month, depending on services billed under CPT codes 99454, 99457, and 99458.
Typical Medicare Reimbursement Ranges
Based on Medicare reimbursement estimates for 2025–2026:
-
99453: $15–$25 (one-time)
-
99454: $40–$60 per month
-
99457: $45–$55 per month
-
99458: $40–$50 per additional 20 minutes
These values demonstrate the financial viability of RPM programs.
Monthly Revenue Potential
A single patient can generate approximately $80 to $120 per month. Scaling this across 100 patients can result in $8,000 to $12,000 in monthly revenue.
Understanding revenue is important, but execution is what ultimately drives success.
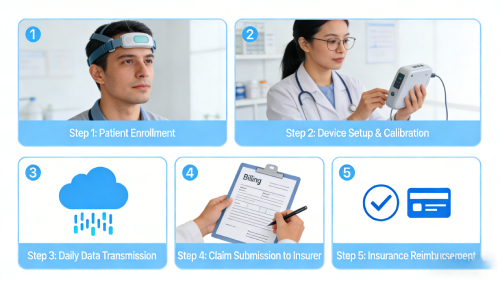
How to Bill RPM Medicare (Step-by-Step Workflow)
A structured workflow ensures compliance and maximizes reimbursement.
Step 1 – Patient Enrollment
Providers must identify eligible patients and obtain documented consent before initiating RPM services.
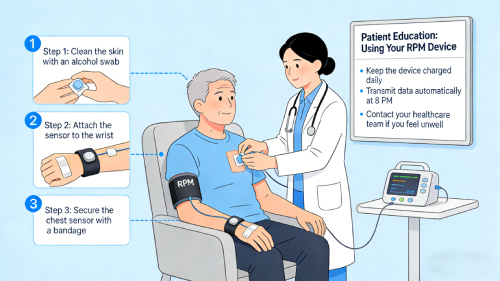
Step 2 – Device Setup (99453)
Devices are installed and patients are trained on how to use them properly.
Step 3 – Data Collection (99454)
Providers must ensure that at least 16 days of data are recorded within each billing cycle.
Step 4 – Monitoring & Communication (99457)
Clinical staff must track time spent reviewing data and communicate with patients through real-time interactions.
Step 5 – Additional Time Billing (99458)
When care exceeds 20 minutes, additional time can be billed to increase reimbursement.
While RPM is highly effective, many providers compare it with other care models.
RPM vs CCM vs Telehealth (Billing Differences Explained)
Understanding how RPM compares to other models helps providers optimize their billing strategy.
RPM vs CCM Billing
RPM relies on device-generated data and continuous monitoring, while Chronic Care Management (CCM) focuses on care coordination without requiring connected devices.
RPM vs Telehealth
RPM involves continuous patient monitoring, whereas telehealth is typically limited to scheduled virtual visits.
Beyond basic billing, there are advanced scenarios that can further increase revenue.
Advanced RPM Billing Scenarios (High-Intent Use Cases)
Can Multiple RPM Codes Be Billed Together?
Yes, providers can bill multiple RPM codes together, such as 99454 and 99457, as long as all requirements are met.
Can RPM and CCM Be Billed Together?
RPM and CCM can be billed together if services are distinct and properly documented.
RPM Billing Frequency Rules
Most RPM codes are billed monthly, provided that all CMS requirements are satisfied during the billing period.
Even experienced providers can make mistakes that impact reimbursement.
Common RPM Billing Mistakes (Avoid CMS Denials)
Not Meeting the 16-Day Requirement
Failure to meet the minimum data requirement is the most common reason for denied claims.
Poor Documentation
Incomplete records can result in compliance issues and failed audits.
Missing Communication Logs
Interactive communication must be documented to bill CPT 99457.
Incorrect Time Tracking
Inaccurate tracking of time spent on patient care can lead to lost revenue.
To better understand RPM’s financial impact, it is helpful to look at a real-world example.
Real Example: RPM Revenue Case Study
Consider a clinic with 50 RPM patients:
-
99454 ($50 average) → $2,500
-
99457 ($50 average) → $2,500
Total monthly RPM revenue: approximately $5,000
Scaling to 100 patients can generate around $10,000 per month, demonstrating the strong ROI of RPM programs.
Finally, here are answers to some of the most frequently asked questions.
FAQs About RPM CPT Codes
Can RPM Be Billed Every Month?
Yes, RPM can be billed monthly as long as all CMS requirements are met.
What Are RPM CPT Code Requirements?
Requirements include the 16-day data rule, proper documentation, time tracking, and interactive communication.
How Much Does RPM Reimburse in 2026?
RPM typically reimburses between $80 and $120 per patient per month.
Is RPM Covered by Medicare?
Yes, RPM is covered under Medicare and supported by CMS guidelines.
Conclusion: Maximize RPM Revenue with Correct Billing
Understanding RPM CPT codes, billing requirements, and Medicare rules is essential for providers looking to scale their remote care programs in 2026.
By following CMS guidelines, optimizing documentation, and implementing a structured workflow, providers can maximize reimbursement and deliver better patient outcomes.
For a broader strategy, explore related resources on remote patient monitoring benefits and RPM program implementation.













