Introduction
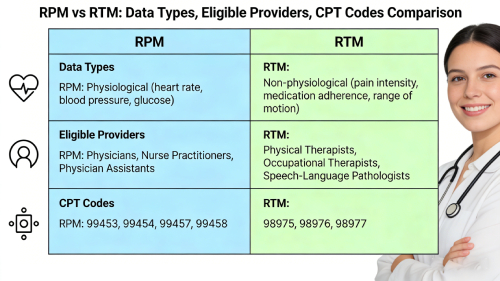
The key difference between RPM and RTM lies in the type of data collected and the providers eligible to bill under CMS rules.
RPM (Remote Patient Monitoring) tracks physiological data—like blood pressure or glucose—through FDA-cleared devices.
RTM (Remote Therapeutic Monitoring) monitors non-physiological therapy data, such as pain, adherence, or mobility, via apps or software, and allows therapists to bill under CMS 2025 guidelines.
In this guide, we break down the RPM vs RTM difference, including CPT codes, billing rules, CMS updates, and when each model works best for your practice.
What Is Remote Patient Monitoring (RPM)?
Definition and Core Purpose
Remote Patient Monitoring (RPM) enables healthcare providers to collect physiological data from patients at home using connected medical devices.
Examples of RPM Data
-
Blood pressure, glucose, heart rate, weight
-
Oxygen saturation and temperature
-
ECG or other biometric readings
RPM helps manage chronic diseases such as hypertension, diabetes, and heart failure.
It’s reimbursable under Medicare’s CMS 2025 Physician Fee Schedule and supports incident-to billing under general supervision.
Explore our complete RPM reimbursement guide for CPT breakdowns and billing workflows.

What Is Remote Therapeutic Monitoring (RTM)?
Definition and Who It’s For
Remote Therapeutic Monitoring (RTM) extends digital care to non-physiological data points like therapy adherence, pain levels, and functional improvement.
Designed For:
-
Physical Therapists (PTs)
-
Occupational Therapists (OTs)
-
Speech-Language Pathologists (SLPs)
RTM enables therapists to monitor rehab progress remotely, helping increase adherence and documentation quality.
RTM is billed through CPT codes 98975–98981, as outlined in the CMS 2025 Fee Schedule.
What Is the Main Difference Between RPM and RTM?
Direct Comparison (Short)
The main difference between RPM and RTM is what they measure and who can bill for them.
-
RPM tracks objective physiological data using FDA-approved devices like blood pressure cuffs or glucose meters.
-
RTM tracks subjective therapeutic data like pain, mobility, or exercise adherence using software or apps.
RPM is billed by physicians and advanced practitioners.
RTM expands eligibility to therapists, including PTs, OTs, and SLPs.
In short, RPM measures vitals; RTM measures function.
RPM vs RTM: Key Differences Explained
Data Type & Source
| Aspect | RPM | RTM |
|---|---|---|
| Data Type | Physiological (vitals, biometrics) | Non-physiological (pain, adherence, function) |
| Data Source | Automatically captured via the device | Patient-reported through apps |
| FDA Device Required | Yes | No |
| Example Data | Blood pressure, glucose | Pain levels, therapy progress |
Device Requirements
-
RPM: Uses FDA-cleared medical devices with automatic transmission.
-
RTM: Relies on digital software or mobile applications that capture patient-reported metrics.
CMS 2025 update: RTM software must provide timestamped data logs to qualify for reimbursement.
Eligible Providers
| Provider Type | RPM | RTM |
|---|---|---|
| Physicians / NPs / PAs | ✅ | ✅ |
| Physical Therapists | ❌ | ✅ |
| Occupational Therapists | ❌ | ✅ |
| Speech Therapists | ❌ | ✅ |
This is a crucial difference between RPM and RTM: RTM expands billing eligibility beyond physicians to therapy professionals.
CPT Codes Comparison (RPM vs RTM CPT Codes 2025)
| Category | RPM Codes | RTM Codes |
|---|---|---|
| Setup & Education | 99453 | 98975 |
| Device / Software Supply | 99454 | 98976–98977 |
| Management (20 min) | 99457 | 98980 |
| Additional 20 min | 99458 | 98981 |
| Supervision Rule (2025) | General | General |
For RPM vs RTM CPT codes, note that RPM requires device data for at least 16 days, while RTM can include self-reported therapy data.
Billing & Reimbursement Differences
| Billing Factor | RPM | RTM |
|---|---|---|
| Billing Cycle | 30 days | 30 days |
| Average Reimbursement | $120–$150 PMPM | $80–$100 PMPM |
| Eligible Providers | MD, NP, PA | PT, OT, SLP |
| Supervision | General | General (CMS 2025 clarified) |
| Incident-To Rules | Allowed | Allowed (per 2025 updates) |
See detailed RPM billing requirements 2025 for implementation steps.
Short Summary: RPM vs RTM at a Glance
-
RPM monitors objective vital signs like BP or glucose with medical devices.
-
RTM monitors subjective therapy data, such as pain or adherence via apps.
-
RPM is billed by physicians, while RTM is billed by therapists.
This 3-line difference format is optimized for Featured Snippet and voice search queries like “What’s the difference between RPM and RTM?”
Can You Bill RPM and RTM Together?
Yes, but only if they track separate data types or conditions.
Example:
-
RPM → Blood pressure monitoring post-stroke
-
RTM → Rehabilitation progress tracking for the same patient
CMS 2025 guidance: No overlapping billing for identical clinical data streams.
When Should You Choose RPM?
Choose RPM if your practice focuses on:
-
Chronic disease management
-
Continuous biometric tracking
-
Preventing readmissions
-
Coordinating chronic care management (CCM)
RPM integrates seamlessly with chronic care reimbursement programs and is ideal for primary care, cardiology, and internal medicine.
When Should You Choose RTM?
Choose RTM if your focus is:
-
Functional recovery and rehab
-
Pain and therapy adherence tracking
-
Outpatient therapy or PT clinics
RTM empowers rehab and therapy practices to extend patient engagement digitally.
RTM for Physical Therapy Practices
RTM for Physical Therapists has become a major growth area since CMS 2022, with enhanced supervision flexibility in 2025.
Core RTM Workflow:
-
Assign digital therapy plan via app
-
Patient logs pain levels and exercise adherence
-
Data automatically syncs to the provider dashboard
-
Therapist reviews ≥20 minutes per month → Bills CPT 98980/98981
Tip: Combine RTM with digital outcomes tracking for insurance justification and MIPS incentives.
Incident-To Billing: RPM vs RTM
Historically, RPM followed incident-to billing under physician oversight.
As of CMS 2025, RTM also allows general supervision, letting therapists delegate technical tasks to auxiliary staff while maintaining compliance.
This change significantly reduces administrative friction for multi-provider organizations.
Practical Workflow Differences
| Stage | RPM Workflow | RTM Workflow |
|---|---|---|
| 1. Enrollment | Patient onboarding & consent | Therapy plan setup & education |
| 2. Data Capture | Device sync (automatic) | Patient self-report via app |
| 3. Review Process | Clinician review & alerts | Therapist review & feedback |
| 4. Billing | 99453–99458 | 98975–98981 |
| 5. Outcomes | Chronic condition tracking | Functional progress tracking |

RPM vs RTM in Value-Based Care
Both models align with value-based reimbursement frameworks by:
-
Reducing readmissions
-
Improving patient adherence
-
Enhancing care continuity
-
Supporting MIPS and ACO quality metrics
Combined use of RPM and RTM creates data-rich hybrid care programs across chronic and rehabilitative domains.
FAQs About RPM and RTM
Q1. What’s the main RPM vs RTM difference?
A1. RPM measures physiological data; RTM tracks therapeutic and functional data.
Q2. Can physical therapists bill RPM?
A2. No, therapists can’t bill RPM but can bill RTM codes (98975–98981).
Q3. What CPT codes are used for RTM in 2025?
A3. RTM uses CPT 98975–98981 under the CMS 2025 Physician Fee Schedule.
Q4. Can I bill RPM and RTM together?
A4. Yes, for distinct conditions with separate documentation.
Q5. What’s “incident-to billing” for RTM?
A5. It allows RTM services to be supervised under general supervision rules.

Conclusion
Understanding the difference between RPM and RTM helps providers choose the right reimbursement strategy.
-
Use RPM for physiological data and chronic condition tracking.
-
Use RTM for therapeutic data and patient adherence tracking.
-
Combine both to unlock full-spectrum remote care.
Many practices generate $100–$150 per patient per month with RPM and $80–$100 via RTM.
See how your organization could scale revenue from compliant remote care.
Read our complete RPM CPT codes guide.